Mpox Prevention & Guidance
Mpox is spread from person to person through close contact like skin-to-skin or face-to-face through:
- Direct contact with infected skin rash, lesions, scabs, or body fluids
- Respiratory droplets during prolonged, face-to-face contact or during intimate physical contact, such as kissing, cuddling, or sex
- Contact with clothing, linens, towels, or other materials contaminated by infectious rash or body fluids
Spread can occur during intimate activities, including:
- Oral, anal, and vaginal sex
- Hugging, kissing, and cuddling
- Contact with bedding or other items that have the virus on them during or after intimate activity
Less frequently, mpox can also spread:
- From a pregnant mother to her fetus through the placenta
- From infected animals to people, either by being scratched or bitten or by preparing or eating infected meat or products. Guidance for pets can be found on the CDC’s website.
At this time, it is not known if mpox can spread through saliva, semen, or vaginal fluids.
Mpox can spread from the time symptoms start until the rash has fully healed and a fresh layer of skin has formed. This process will vary from person to person but typically takes about 2-4 weeks.
Anyone, regardless of sexual orientation or gender identity can get mpox through close, personal contact with someone who has symptoms of mpox. However, data suggests the virus has primarily spread through close-knit social networks of gay, bisexual, and other same gender-loving men through intimate contact. Risk is especially high for same gender-loving men who have multiple or anonymous sexual partners.
Take the following steps to prevent getting mpox:
- Get vaccinated if you meet the eligibility criteria, and make sure to get the second recommended does 28 days later.
- Avoid close skin-to-skin contact with people who have a rash that looks like mpox.
- Do not touch the rash or scabs of someone with mpox.
- Do not kiss, hug, cuddle, or have sex with someone with mpox.
- Avoid contact with objects and materials that a person with mpox has used.
- Do not share food, drinks, or eating utensils with someone with mpox.
- Do not handle or touch the bedding, towels, or clothing of someone with mpox.
- Wash your hands often with soap and water or use an alcohol-based hand sanitizer.
If you or your partners are sick:
- Do not have sex or close physical contact, especially if you or they have a rash or sore, until you have talked to a healthcare provider.
- If you choose to have sex while sick, avoid kissing and other face-to-face contact. Cover all sores with clothing or bandages to help reduce risk of spread.
- Wash your hands, sex toys, and bedding before and after sex.
Evaluate the level of risk when making plans or deciding whether to attend certain events:
- Having sex or other intimate contact with multiple or anonymous people, such as those met through dating apps or on social media, increases your risk of exposure.
- Clubs, raves, saunas, sex parties, and other events may also increase your risk of exposure, especially if people are wearing less clothing.
Frequently Asked Questions
Mpox (monkeypox) is a viral infection, with symptoms that can include a painful and uncomfortable rash or sores, often accompanied with flu-like illness. Mpox is rarely fatal. The virus is part of the same family of viruses that causes smallpox, and symptoms are similar to smallpox symptoms, but milder. Mpox is not related to chickenpox.
Several countries where mpox is not common have reported cases since May 2022 and there have been confirmed cases in almost every state in the United States. Most of the infected individuals have reported only mild symptoms, but one person has died. Additional cases are being investigated. Updated case counts by state can be found at the CDC’s 2022 U.S. Map & Case Count. Updated Chicago case totals can be found at the CDPH Mpox Data Dashboard.
In this outbreak, skin-to-skin contact with infectious skin lesions during intimate sexual activity (e.g., oral, anal, and vaginal sex or touching the genitals or anus) may be the likely mode of transmission. Studies are underway in affected countries to determine the source of infection of each identified case, and actions are being taken to provide medical care and limit further spread.
The most common symptom is a rash or sores that look like pimples or blisters. The rash may appear on one part of the body or across the body, including on the face, inside the mouth, in the genital and anal regions, chest, hands, and feet. The rash or sores can be mild, but also can be extremely painful and itchy and may interfere with normal activities.
Some people may have flu-like symptoms, including fever, chills, fatigue, and swollen glands or lymph nodes that occur before or at the same time as the rash and sores.
Mpox symptoms usually start several days to 2 weeks after exposure but may not appear for up to 21 days. The virus can spread from the time symptoms start until the rash has fully healed and a fresh layer of skin has formed. This process will vary from person to person but typically takes about 2-4 weeks.
If you think you have symptoms that could be mpox, seek advice from your health care provider.
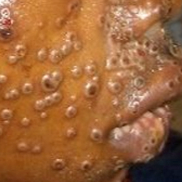
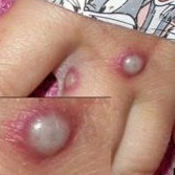
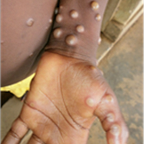
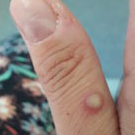
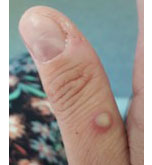
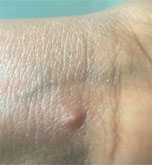
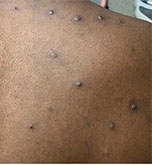

Photo Credit: NHS England High Consequence Infectious Diseases Network
Mpox may spread from person to person through close contact like skin-to-skin or face-to-face through:
- Direct contact with infected skin rash, lesions, scabs, or body fluids
- Respiratory droplets during prolonged, face-to-face contact or during intimate physical contact, such as kissing, cuddling, or sex
- Contact with clothing, linens, towels, or other materials contaminated by infectious rash or body fluids
Spread can occur during intimate activities, including:
- Oral, anal, and vaginal sex
- Hugging, kissing, and cuddling
- Contact with bedding or other items that have the virus on them during or after intimate activity
Less frequently, mpox can also spread:
- From a pregnant mother to her fetus through the placenta
- From infected animals to people, either by being scratched or bitten or by preparing or eating infected meat or products. Guidance for pets can be found on the CDC’s website.
At this time, it is not known if mpox can spread through saliva, semen, or vaginal fluids.
Mpox can spread from the time symptoms start until the rash has fully healed and a fresh layer of skin has formed. This process will vary from person to person but typically takes about 2-4 weeks.
Mpox can spread from one person to another through close physical contact, including sexual contact. Mpox can more accurately be described as “sexually transmissible.” In other words, sex is just one of the ways that mpox can be spread.
Mpox rashes are sometimes found on genitals and in the mouth, which is likely to contribute to transmission during sexual contact. Mouth-to-skin contact could also cause transmission where skin or mouth lesions are present.
Mpox rashes can resemble some sexually transmitted diseases, including herpes and syphilis.
Ask your sex partners about symptoms. See if they have had any unusual rashes and sores in the last 3 weeks.
The risk of becoming infected with mpox is not limited to people who are sexually active or gay, bisexual, or other same gender-loving men. Anyone who has close physical contact with someone who is infectious is at risk. Anyone who has symptoms that could be mpox should seek advice from a health worker immediately.
Anyone who has close physical contact with someone who has symptoms of mpox.
Even though people who have been vaccinated against smallpox will have some protection against mpox, they also need to take precautions to protect themselves and others.
Newborns, children, and people with underlying immune deficiencies may be at risk of more serious symptoms and death from mpox.
Anyone, regardless of sexual orientation or gender identity, can get mpox through close, personal contact with someone who has symptoms of mpox. However, data suggests that the virus has primarily spread among social networks of gay, bisexual, and same gender-loving men through intimate contact. Risk is especially high for same gender-loving men who have multiple or anonymous sexual partners.
Take the following steps to prevent getting mpox:
- Get vaccinated if you meet the eligibility criteria.
- Avoid close skin-to-skin contact with people who have a rash that looks like mpox.
- Do not touch the rash or scabs of someone with mpox.
- Do not kiss, hug, cuddle, or have sex with someone with mpox.
- Avoid contact with objects and materials that a person with mpox has used.
- Do not share food, drinks, or eating utensils with someone with mpox.
- Do not handle or touch the bedding, towels, or clothing of someone with mpox.
- Wash your hands often with soap and water or use an alcohol-based hand sanitizer.
Evaluate the level of risk when making plans or deciding whether to attend certain events:
- Having sex or other intimate contact with multiple or anonymous people, such as those met through dating apps or on social media, increases your risk of exposure.
- Clubs, raves, saunas, sex parties, and other events may also increase your risk of exposure, especially if people are wearing less clothing.
Yes. The JYNNEOS™ vaccine can help protect people against mpox when given before or soon after exposure to the virus. CDPH strongly encourages those eligible to get the vaccine to protect themselves and others. The vaccine is a two-dose vaccine given 28 days apart. Optimal protection is not achieved until two weeks following the second dose.
The two-dose series of mpox vaccine is currently available to anyone who:
- Lives in Chicago and Illinois, including students enrolled in Chicago’s universities/colleges
- Has not previously been infected with mpox
The vaccine is recommended for those who are or anticipate:
- Having had skin-to-skin or intimate contact (e.g., household members with close physical contact or intimate partners) with someone diagnosed with mpox
- Living with HIV, especially those with uncontrolled or advanced HIV
- Being eligible for or currently taking HIV-PrEP
- Exchanging good or services for sex
- Being a sexually active bisexual, gay or other same gender-loving man, or sexually active transgender individuals. Especially consider getting vaccinated if you:
- Meet recent partners through online applications or social media platforms (such as Grindr, Tinder or Scruff), or at clubs, raves, sex parties, saunas
- Are diagnosed with sexually transmitted infection(s) (STI) in the past 6 months
If you are eligible to receive the mpox vaccine, contact your healthcare provider or see the list of vaccine providers below. Encourage your healthcare provider to visit Chicago Health Alert Network if they are unfamiliar with mpox. The Chicago healthcare providers listed here have received doses of vaccine for those who meet eligibility criteria. Please contact the providers directly to see if they have currently available doses or appointments.
- Review how mpox spreads and whether you have had close contact with someone who has been diagnosed with mpox.
- Practice good prevention.
- Continue routine daily activities (e.g., school, work) as long as you do not have symptoms but avoid close, personal, skin-to-skin contact
- Avoid sex and other close personal contact
- Avoid large gatherings, especially if they involve close, personal, skin-to-skin contact
- Do not share personal items like towels, bedding, dishes, utensils, or eating utensils
- Get vaccinated. The mpox vaccine is recommended for anyone, regardless of sexual orientation or gender identity, who has been in close, personal contact with someone who has been diagnosed with mpox. Vaccinations can reduce the risk of infection and serious illness for those who have been exposed but are not exhibiting symptoms. Make sure to get the second recommended does 28 days later.
- Watch for signs and symptoms for 21 days from the date of your last exposure.
- Take your temperature with a thermometer twice a day (morning and night)
- Check for rash or unusual sores that look like pimples or blisters on the face, body, and genitals
- Call your healthcare provider or a health center if you show symptoms or need to be evaluated or tested. There is no at-home test for mpox. The test can only be given to those exhibiting rash symptoms. If you don’t have a doctor or insurance, contact HIV/STI Resource Hub at 844.482.4040/hivhub.org or visit FindAHealthCenter.hrsa.gov for free or low-cost care.
- Isolate if you or your partner(s) feel sick or have a new or unexplained rash or sores.
- Isolate in a private room and avoid close contact with other people and animals in your household.
- Take a break from sex and other close personal contact.
- Do not share personal items like towels, bedding, dishes, utensils, or eating utensils.
- Use a face mask and cover rash and sores when you are unable to separate from others.
- Call your health care provider or a health center right away if you or your partner(s) show signs and symptoms of mpox. If you don’t have a doctor or insurance, contact HIV/STI Resource Hub at 844.482.4040 / hivhub.org or visit FindAHealthCenter.hrsa.gov for free or low-cost care.
- Get tested through your healthcare provider. There is no at-home test for mpox. The test can only be given to those exhibiting rash symptoms.
- Let close contacts know that they may have been exposed to mpox. Communication is the key to controlling this outbreak.
- Take care of yourself and follow recommended treatments. Most people with mpox recover fully within 2 to 4 weeks without the need for medical treatment.
Currently, testing is only recommended if you have a rash consistent with mpox. Your healthcare provider will help you decide if you need to be tested for mpox. There is no at-home test for mpox. There is no test for mpox for those not exhibiting symptoms.
If you have been tested and diagnosed with mpox, you will be required to isolate at home.
While you are isolating, you should not leave your home unless it is required for medical care. If you need to seek healthcare while you are isolating, please call your doctor’s office or hospital in advance to let them know you have been diagnosed with mpox.
- Isolate in a private room and avoid close contact with other people and animals in your household
- Take a break from sex and other close personal contact
- Do not share personal items like towels, bedding, dishes, utensils, or eating utensils
- Use a face mask and cover rash and sores when you are unable to separate from others
Your isolation can end when all lesions have resolved, all scabs have fallen off, and a fresh layer of intact skin has formed. This process will vary from person to person but typically takes about 2-4 weeks. Individuals with mpox should contact their healthcare provider to determine if it is appropriate to end isolation.
Mpox is a potentially serious viral illness; however, the United States has ways to respond to its emergence. Chicago Department of Public Health (CDPH) continues to support clinical partners with testing to identify infected individuals, isolate anyone found to be infected with the virus, trace infected individuals' close contact with others, and monitor for symptom onset during the incubation period. In collaboration with federal partners, CDPH coordinates post exposure prophylaxis of exposed contacts as well as treatment with antiviral medication for those with more severe illness.




