Mpox Symptoms & Treatment
If you think you have symptoms that could be mpox (monkeypox), seek advice from your healthcare provider.
- Call ahead to your doctor’s office or hospital to let them know that you may have mpox.
- Cover all parts of the rash with clothing, gloves, or bandages
- Wear a mask
- Let your healthcare provider know if you have had close contact with someone who has suspected or confirmed mpox.
- Encourage your healthcare provider to visit Chicago Health Alert Network if they are unfamiliar with mpox
If you don’t have a doctor or insurance, contact HIV/STI Resource Hub at 844.482.4040 / hivhub.org or visit FindAHealthCenter.hrsa.gov for free or low-cost care.
Do not touch or scratch the rash. This can spread the rash to other parts of your body, increase the chance of spreading the virus to others, and possibly cause open lesions to become infected by bacteria.
Signs & Symptoms
Mpox symptoms usually start several days to 2 weeks after exposure but may not appear for up to 21 days. The virus can spread from the time symptoms start until the rash has fully healed and a fresh layer of skin has formed. This process will vary from person to person but typically takes about 2-4 weeks.
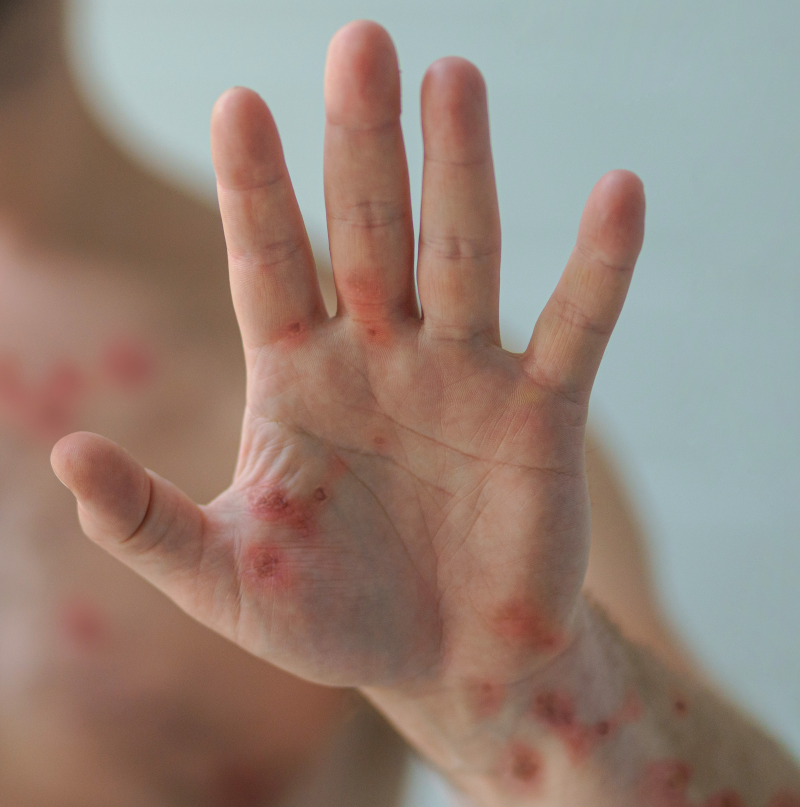
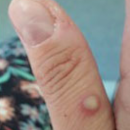
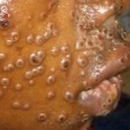
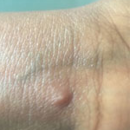
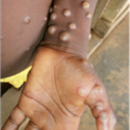
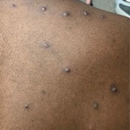
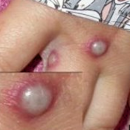
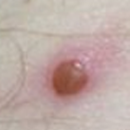
The most common symptom is a rash or sores that look like pimples or blisters. The rash may appear on one part of the body or across the body, including on the face, inside the mouth, in the genital and anal regions, chest, hands, and feet. The rash or sores can be mild, but also can be extremely painful and itchy and may interfere with normal activities.
Some people may have flu-like symptoms, including fever, chills, fatigue and swollen glands or lymph nodes that occur before or at the same time as the rash and sores. Complications can occur, including proctitis (inflammation of the lining of the rectum) or scarring from sores that may affect the ability to urinate or defecate. If you think you have symptoms that could be mpox, seek advice from your health care provider.

Testing
Currently, testing is only available if you have a rash consistent with mpox. Your healthcare provider will help you decide if you need to be tested for mpox. There is no at-home test for mpox. There is no test for mpox for those not exhibiting symptoms.
Your healthcare provider may take a specimen and send it to a lab for testing. Results are usually available within a few days. While you are waiting for your results, take precautions to avoid getting or spreading mpox virus to others.
Isolation
If you have been tested and diagnosed with mpox, you will be required to isolate at home until all your rash lesions have resolved, the scabs have fallen off, and a fresh layer of skin has formed. This process will vary from person to person but typically takes about 2-4 weeks. Individuals with mpox should contact their healthcare provider to determine if it is appropriate to end isolation.
While you are isolating, you should not leave your home unless it is required for medical care. If you need to seek healthcare while you are isolating, please call your doctor’s office or hospital in advance to let them know you have been diagnosed with mpox.
- Isolate in a private room and avoid close contact with other people and animals in your household
- Avoid visits from anyone who is not essential in your home
- Take a break from sex and other close personal contact
- Avoid shaving areas of the body with lesions as this can lead to spread of the virus
- Avoid use of contact lenses to prevent inadvertent infection of the eye
- Do not share personal items like towels, bedding, dishes, utensils, or eating utensils
- Use a face mask and cover rash and sores when you are unable to separate from others
- Wear a condom for 8 weeks after recovering from mpox.
Treatment
Many people with mpox recover fully within 2 to 4 weeks without any medical treatment, but some patients benefit from either supportive care to control discomfort such as pain or itching or through treatment with a medication called Tecovirimat (TPOXX).
Ways to make yourself more comfortable if you have mpox:
- There are no treatments specifically for mpox. But because the viruses that cause mpox and smallpox are similar, antiviral drugs developed to protect against smallpox may be used to treat monkeypox effectively.
- Drink plenty of water and other clear fluids to prevent dehydration.
- Keep sores clean and dry when not showering or bathing to prevent bacterial infections.
- Avoid touching or scratching the rash. This can spread the rash to other parts of your body, increase the chance of spreading the virus to others, and possibly cause open lesions to become infected by bacteria.
- Manage itching with over-the-counter oral antihistamines (such as diphenhydramine/Benadryl, cetirizine or hydroxyzine) or topical ointments such as calamine lotion or petroleum jelly (Vaseline).
Discuss treatment options with a healthcare provider if you are having pain in the mouth, genital region, or anus, nausea/vomiting, diarrhea, or difficulty urinating or defecating. Providers may prescribe different medications depending on your symptoms:
- Mouth pain or sores: “Magic or miracle mouthwash” or antiseptic oral rinses to decrease mouth pain and keep sores clean. Topical over-the-counter oral gels to reduce pain, such as Orajel, can be used in limited doses but should be discussed with a healthcare provider.
- Painful sores in the genital and anal regions: warm sitz baths. Topical pain-relief gels or creams (e.g., RectiCare) may also provide temporary relief. Please note: if you have blood in your urine, difficulty urinating, inability to retract your foreskin, or your foreskin can’t return to a normal position after being retracted, contact a healthcare provider immediately.
- Proctitis (swelling and inflammation of the lining of the rectum internal to the anus): stool softeners such as docusate and warm sitz baths. Over the counter pain medications such as acetaminophen can also be used. Additional prescription pain medications might also be necessary, but side effects should be discussed with a healthcare provider. Please note: if you are unable to pass a bowel movement or have blood in your stool, contact a healthcare provider immediately.
- Nausea/vomiting: prescription medications to control nausea.
- Diarrhea: fluid and electrolyte replacement. Over-the-counter medications are not recommended.
- Bacterial infections: antibiotics as needed.
Mpox can occur at the same time as other sexually transmitted infections such as gonorrhea, syphilis, chlamydia, and HIV, so your healthcare provider may also evaluate and treat you for other infections.




